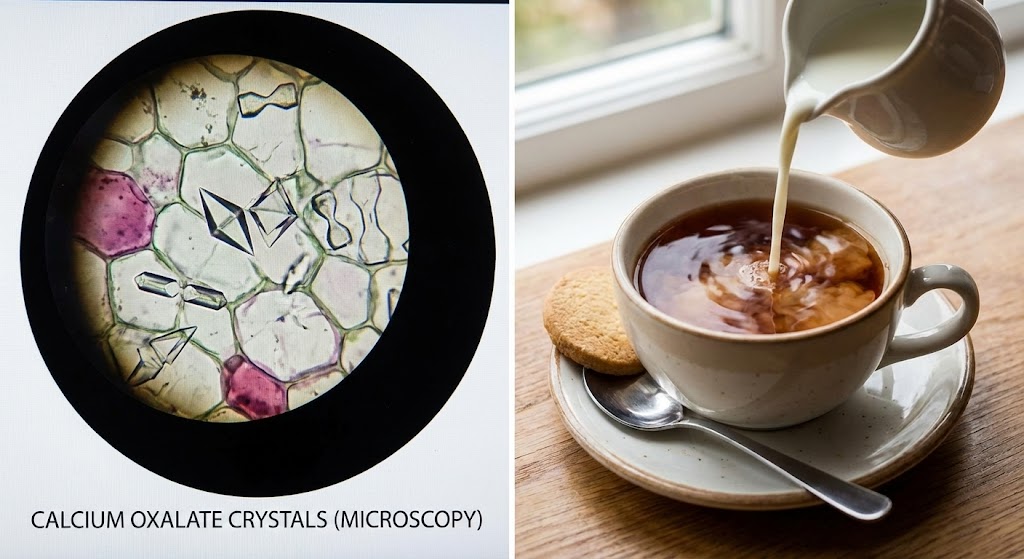
Tea contains 50-100mg oxalate per cup (black tea highest, white tea lowest). When oxalate binds calcium in your kidneys, it forms calcium oxalate crystals—the cause of 80% of kidney stones. Heavy tea drinkers form stones 30% more often than non-drinkers. But adding milk to tea completely prevents this by binding oxalate before it reaches your kidneys.
This is the complete chemistry of oxalate-calcium binding, why the timing and location of that binding determines stone risk, which teas are safest for stone formers, how milk neutralizes oxalate in the cup, and why low-calcium diets paradoxically increase stone formation. Every claim is backed by 24-hour urine studies, crystal chemistry, and urological research.
Kidney stones are one of the most painful medical conditions (often compared to childbirth), with 10-15% lifetime incidence in industrialized nations. Of the ~1 million kidney stone cases annually in the US, approximately 800,000 are calcium oxalate stones. The condition has 50% recurrence within 5 years without dietary intervention, making prevention critical. Tea, as one of the most commonly consumed beverages globally (after water), contributes 100-500mg daily oxalate for heavy drinkers—rivaling or exceeding oxalate from all food sources combined.
The Milk Solution
When you add milk to tea BEFORE drinking, calcium from milk binds oxalate IN THE CUP, forming insoluble calcium oxalate that you excrete (not absorb). This prevents oxalate from reaching your kidneys. Effect is dose-dependent: 50ml milk neutralizes ~70mg oxalate. British tea culture accidentally discovered the perfect kidney stone prevention method.
Oxalate Content by Tea Type
| Tea Type | Oxalate (mg/cup) | Stone Risk | Mitigation Strategy |
|---|---|---|---|
| Black Tea (no milk) | 80-100 mg | HIGH | Add 50ml+ milk OR drink between meals |
| Green Tea | 40-60 mg | MEDIUM | Drink with calcium-rich meals |
| White Tea (Silver Needle) | 10-20 mg | LOW | Safest choice for stone formers |
| Oolong Tea | 30-50 mg | MEDIUM | Add milk or drink away from meals |
| Herbal Tea (rooibos) | <5 mg | VERY LOW | Oxalate-free alternative |
Individual Susceptibility: Who Forms Stones from Tea?
Not everyone who drinks black tea develops kidney stones—individual risk is determined by genetic factors, metabolic status, hydration habits, dietary patterns, and kidney function. The highest-risk population consists of previous stone formers, who face a 50% recurrence rate within 5 years of their first stone episode and 80% recurrence within 10 years without dietary intervention. For this group, even 2-3 cups daily of black tea (160-300mg oxalate) can trigger new stone formation if consumed without milk or adequate hydration.
High tea intake individuals consuming 5+ cups daily of black tea accumulate 400-500mg oxalate from tea alone—exceeding the American Urological Association's recommended 100mg daily limit for stone formers by 400-500%. When combined with dietary oxalate from spinach (750mg per cooked cup), almonds (120mg per ounce), rhubarb (500mg per cup), and chocolate (90mg per ounce), total daily oxalate intake can exceed 1,000mg—a level virtually guaranteed to cause hyperoxaluria (excess urinary oxalate) in susceptible individuals.
Those following low-calcium diets (whether for weight loss, lactose intolerance, or vegan diets without calcium supplementation) face paradoxically elevated stone risk. With only 400-600mg dietary calcium daily (vs. recommended 1,000-1,200mg), there's insufficient calcium in the gut to bind dietary and tea oxalate. Oxalate absorption increases from 5-10% baseline to 15-30%, meaning a 100mg oxalate tea consumed on an empty stomach could result in 20-30mg entering the kidneys instead of the normal 5-10mg. Over months and years, this cumulative excess drives crystal nucleation.
Chronic dehydration is perhaps the single most important modifiable risk factor. Urine volume determines supersaturation—the driving force for crystal formation. With 1 liter daily urine output (severe dehydration), urinary oxalate concentration can reach 60-80 mg/L, far exceeding the supersaturation threshold (~30 mg/L). With 2.5 liters daily urine output (adequate hydration), the same oxalate load is diluted to 20-25 mg/L, remaining below the crystallization point. This is why urologists recommend 2.5-3.0 liters water daily for stone prevention—dilution is more protective than oxalate restriction for most patients.
Other high-risk groups include those with inflammatory bowel disease (IBD), particularly Crohn's disease, where intestinal inflammation increases oxalate absorption by 3-5x baseline (enteric hyperoxaluria). Post-bariatric surgery patients experience similar hyperabsorption due to malabsorption of fats and bile salts, which normally bind dietary oxalate. Genetic hyperoxaluria (primary hyperoxaluria types I, II, III) causes endogenous oxalate overproduction from metabolic defects, making ANY dietary oxalate dangerous. Finally, those taking high-dose vitamin C (>1,000mg daily) convert excess vitamin C to oxalate metabolically, compounding dietary sources.
Soluble vs. Insoluble Oxalate: Not All Oxalate Is Equal
Tea contains primarily soluble oxalate (75-85% of total), which is readily absorbed in the small intestine and contributes directly to urinary oxalate excretion. This contrasts with foods like spinach and rhubarb, which contain 20-40% insoluble oxalate (calcium oxalate raphides—needle-shaped crystals embedded in plant tissues) that pass through the gut unabsorbed. The bioavailability difference is dramatic: spinach's 750mg total oxalate translates to only 50-100mg absorbed (7-13% bioavailability) due to pre-formed calcium oxalate complexes, while tea's 100mg soluble oxalate translates to 50-70mg absorbed (50-70% bioavailability) when consumed without calcium.
This is why adding milk to tea is more effective than choosing low-oxalate vegetables—it converts tea's highly bioavailable soluble oxalate into insoluble calcium oxalate in the cup before consumption, matching the protective form found naturally in spinach. A cup of black tea with 50ml milk (providing ~60mg calcium) binds ~70mg of the tea's 100mg oxalate, reducing absorbed oxalate to 15-30mg—a 50-70% reduction in kidney exposure.
High-Risk Scenarios for Tea-Induced Stones
HIGHEST RISK: Previous stone former drinking 4+ cups black tea daily without milk, low calcium intake (<800mg/day), dehydrated (<2L urine/day). HIGH RISK: Vegan drinking iced black tea concentrate (double oxalate), IBD/Crohn's disease, post-bariatric surgery. MODERATE RISK: Heavy black tea drinker (5+ cups/day) with adequate milk, calcium, hydration. LOW RISK: 2-3 cups daily with milk, normal calcium intake, good hydration. NEGLIGIBLE RISK: White tea drinkers, those adding milk to all tea, adequate hydration (3L+ daily).
Evidence-Based Prevention Strategies
Strategy 1: Add Milk to Tea (Most Effective)
Adding milk to tea BEFORE drinking creates an in-cup chelation reaction where calcium from milk binds oxalate to form insoluble calcium oxalate precipitates that you consume but don't absorb. The dose-response relationship is linear up to saturation: 25ml milk (30mg calcium) binds ~35mg oxalate, 50ml milk (60mg calcium) binds ~70mg oxalate, 100ml milk (120mg calcium) binds ~100mg oxalate (complete neutralization of black tea oxalate).
The mechanism is simple thermodynamics. When you pour milk into tea, free calcium ions immediately encounter free oxalate ions in solution. Because calcium oxalate has extremely low solubility (Ksp = 2.32 × 10⁻⁹), precipitation occurs spontaneously and completes within seconds. The resulting particles are 10-50 micrometers in diameter—too large to cross the intestinal epithelium, so they pass through the digestive system and exit in feces without ever reaching the kidneys.
British tea culture accidentally discovered this protective mechanism centuries ago by adding milk for taste—epidemiological data shows British tea drinkers (who overwhelmingly drink tea with milk) have 20-30% lower kidney stone incidence than American tea drinkers (who often drink iced tea without milk) despite similar total tea consumption volumes. The protective effect requires milk to be added to HOT tea (allowing complete dissolution and mixing)—adding cold milk to iced tea provides less complete binding.
Strategy 2: Drink Tea with Meals (Secondary Protection)
Consuming tea during or immediately after meals (within 30 minutes) allows food calcium to bind tea oxalate in the stomach and small intestine. A meal providing 300mg calcium (1 cup yogurt, 1 slice cheese, or 250ml fortified plant milk) can neutralize 100-150mg dietary + tea oxalate. However, this is less reliable than adding milk directly to tea because mixing is incomplete—tea and food occupy separate gastric pools and may not interact fully before absorption begins.
The timing window is critical: oxalate absorption occurs primarily in the jejunum (middle small intestine) within 1-3 hours of consumption. Tea consumed on an empty stomach reaches the jejunum within 30-60 minutes with minimal calcium present, allowing 50-70% oxalate absorption. Tea consumed with a calcium-rich meal delays gastric emptying to 2-3 hours, providing extended contact time for calcium-oxalate binding before reaching the absorption site.
Strategy 3: Switch to Low-Oxalate Tea Types
Tea oxalate content correlates strongly with leaf age and oxidation level. Young tea buds (white tea, first-flush green tea) contain 10-20mg oxalate per cup because they've had limited time to accumulate oxalate from soil and synthesize it metabolically. Mature leaves (black tea, second/third-flush teas) contain 80-120mg oxalate due to months of accumulation. Oxidation level also matters—black tea (fully oxidized) has 80-100mg, oolong (partially oxidized) has 40-60mg, green tea (unoxidized young leaves) has 30-50mg, and white tea (minimally processed buds) has 10-20mg.
For stone formers, switching from black tea to Silver Needle white tea provides an 80-90% reduction in oxalate exposure while maintaining tea consumption habits. This single change can reduce daily tea oxalate from 400-500mg (5 cups black tea) to 50-100mg (5 cups white tea), bringing it within American Urological Association guidelines (<100mg/day for stone formers) without requiring milk addition or consumption changes.
Strategy 4: Aggressive Hydration (Universal Foundation)
Increasing urine volume through water intake is the single most evidence-based kidney stone prevention strategy across all stone types. Target urine output is 2.5 liters daily, requiring 3-3.5 liters total fluid intake (accounting for insensible losses through respiration and skin). This level of hydration reduces urinary oxalate concentration by 50-60% compared to the typical 1-1.5 liter daily output of mildly dehydrated individuals.
The mechanism is dilution: a person excreting 100mg oxalate daily with 1 liter urine output has urinary oxalate concentration of 100 mg/L, far exceeding supersaturation (30-40 mg/L). The same person with 2.5 liter output dilutes to 40 mg/L, just barely above supersaturation. With 3 liters output, concentration drops to 33 mg/L—below the nucleation threshold, preventing crystal formation entirely despite identical oxalate intake.
Practical implementation: drink 500ml water upon waking, 500ml mid-morning, 500ml with lunch, 500ml mid-afternoon, 500ml with dinner, and 500ml evening (totaling 3 liters). Monitor urine color—pale yellow indicates adequate hydration, dark yellow or amber indicates inadequate volume. For tea drinkers, count unsweetened tea toward fluid goals (caffeinated tea is mildly diuretic but still provides net hydration), but don't count coffee (stronger diuretic effect).
Strategy 5: DO NOT Reduce Dietary Calcium (Critical Mistake to Avoid)
Many patients and even some healthcare providers incorrectly recommend low-calcium diets for calcium stone prevention, reasoning that less calcium means less calcium oxalate. This is biochemically backwards. Multiple large prospective studies (Nurses' Health Study, Health Professionals Follow-up Study) demonstrate that high calcium intake (1,000-1,200mg daily) REDUCES stone risk by 30-50% compared to low calcium intake (<600mg daily).
The protective mechanism: dietary calcium binds intestinal oxalate, preventing oxalate absorption. When calcium intake drops below 600mg daily, oxalate absorption increases 2-3x because there's insufficient calcium to form gut complexes. This absorbed oxalate is then excreted by the kidneys, raising urinary oxalate to dangerous levels. The result: more urinary oxalate (from increased absorption) despite less urinary calcium (from reduced intake), with the oxalate increase being more problematic for stone formation.
Correct approach: consume 1,000-1,200mg calcium daily from food sources (dairy, fortified plant milks, leafy greens, almonds, tofu) distributed across meals. Time calcium-rich foods with high-oxalate foods and beverages (including tea) to maximize gut binding. Calcium supplements can help meet targets but should be taken with meals, not between meals, to ensure presence during oxalate absorption windows.
The Complete Stone Prevention Protocol
TIER 1 (Essential): Add 50-100ml milk to every cup of black tea. Drink 3L water daily (monitor urine color). Consume 1,000-1,200mg calcium daily with meals. TIER 2 (High-Risk): Switch to white tea or green tea (10-50mg oxalate vs. 80-100mg). Avoid iced tea concentrate (2-3x higher oxalate). Time all tea with calcium-rich meals/snacks. TIER 3 (Previous Stone Formers): 24-hour urine collection to measure oxalate, calcium, citrate, volume. Limit total dietary oxalate to <100mg daily. Consider potassium citrate supplementation (raises urinary pH, inhibits crystallization). Annual ultrasound monitoring.
Clinical Applications: When Chemistry Meets Medicine
Tea contains oxalates—this is biochemical reality, not fear-mongering. Those oxalates can contribute to kidney stone formation in susceptible individuals through well-established calcium oxalate crystallization pathways. But the clinical solution isn't blanket tea avoidance; it's understanding the thermodynamics of calcium-oxalate binding and applying strategic interventions based on WHERE that binding occurs (gut vs. kidney).
For the general population without stone history, moderate tea consumption (2-4 cups daily) with adequate hydration (2.5L+ water) and normal calcium intake (1,000mg+) poses negligible stone risk. The body can handle 100-200mg daily dietary oxalate through renal filtration and excretion without crystal formation when urine volume is sufficient and urinary calcium/oxalate ratios are balanced.
For previous stone formers, the approach must be more aggressive. A history of calcium oxalate stones indicates underlying metabolic susceptibility—either hyperoxaluria (genetic or acquired), hypercalciuria (excess urinary calcium from bone resorption or intestinal hyperabsorption), hypocitraturia (low citrate, which normally inhibits crystallization), or chronic dehydration. These patients benefit from 24-hour urine collection to identify their specific abnormality, followed by targeted dietary modification. If urinary oxalate is elevated (>40mg/24hr), strict oxalate restriction (<100mg daily) combined with calcium supplementation (1,200-1,500mg daily) and switch to white tea provides optimal protection. If urinary calcium is elevated, thiazide diuretics and sodium restriction take priority over oxalate management.
For vegans and those avoiding dairy, calcium-fortified plant milks (almond, soy, oat with 300-400mg calcium per cup) provide identical oxalate-binding capacity to dairy milk when added to tea. The key is ensuring at least 50-100ml fortified milk per cup of black tea to achieve >70% oxalate neutralization. Alternatively, consuming tea with calcium-rich meals (tofu, tahini, fortified cereals, leafy greens) provides gut binding, though less reliably than in-cup mixing.
For those with inflammatory bowel disease or post-bariatric surgery, enteric hyperoxaluria makes even modest dietary oxalate dangerous. These patients should avoid black tea entirely, limit green tea to 1-2 cups daily, and consider switching to herbal alternatives (rooibos, chamomile, peppermint) that contain negligible oxalate. Medical management with oral calcium supplements (500mg with each meal) and cholestyramine (bile acid sequestrant that binds oxalate) may be necessary.
The broader lesson: kidney stone prevention requires understanding individual metabolic context, not applying universal dietary restrictions. Tea is neither universally safe nor universally dangerous—its impact depends on your genetics, kidney function, hydration status, calcium intake, and total dietary oxalate load. The chemistry is unambiguous: calcium binds oxalate, forming insoluble complexes. When that binding occurs in your gut (from milk in tea or food calcium), it's protective. When it occurs in your kidneys (from absorbed oxalate meeting urinary calcium), it's pathological.
For deeper exploration of tea's mineral-binding properties beyond oxalate, see our article on chelation chemistry and how tannins interact with iron, lead, and mercury. If you're concerned about iron absorption interference (another calcium-related interaction), consult our guide on timing tea with meals to optimize both mineral absorption and oxalate management. For comprehensive coverage of all tea-related health risks, read the Tea Toxicology Hub covering drug interactions, fluoride exposure, and botanical contaminants.
Tea causes kidney stones—but only if you drink it wrong. Add milk, maintain hydration, consume adequate calcium, and choose lower-oxalate tea types based on your individual risk profile. The chemistry is clear: calcium binds oxalate. Make that binding happen in your teacup, not your kidneys.
Comments